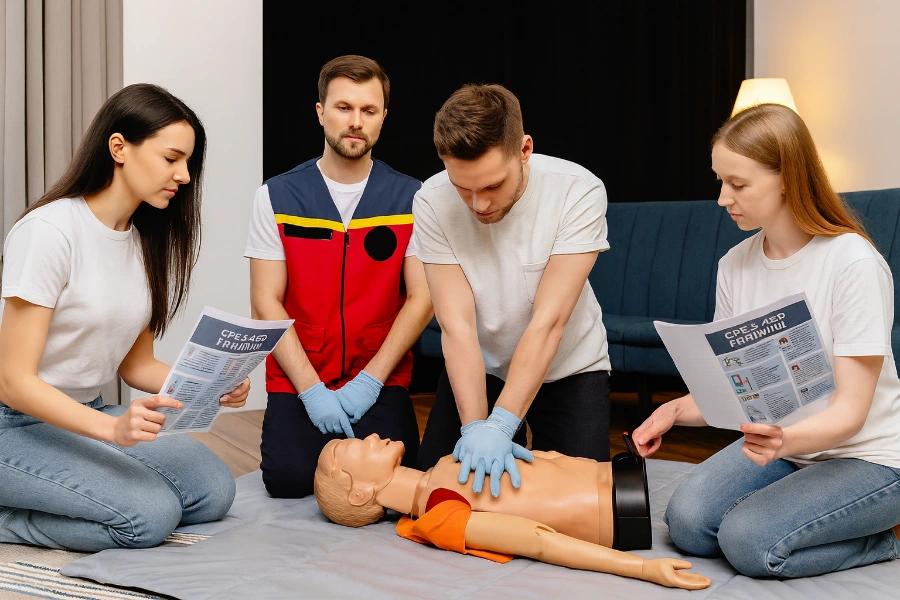
Why summer is the stress test for EMS core skills
Summer brings warmer weather, increased outdoor activity and more people near water or in public venues. These conditions often trigger spikes in trauma, cardiac emergencies, drownings, and heat-related illness. Busy traffic and vacation travel can delay hospital access, making prompt prehospital care more critical than ever. Seasonal surges expose weaknesses in EMS readiness, so crews require sharpened core competencies before demand increases. Recent research shows essential lifesaving skills degrade over time if not practiced regularly, so pre-summer refreshers make strong sense.
Skill #1: High-performance CPR and defibrillation that actually changes survival
What “high-quality” CPR means in current evidence
Guidelines from the American Heart Association (AHA) define high-quality CPR by precise metrics. Rescuers should deliver compressions at 100–120 per minute with a depth of at least 2.0 inches (5 cm). According to the AHA High-Quality CPR guidelines, rescuers must allow full chest recoil, avoid excessive ventilation, and minimize interruptions. Chest compression fraction (the proportion of time spent compressing) should exceed 80%. Data confirm that guideline-compliant compression depth and fraction improve return of spontaneous circulation and survival outcomes. This is reinforced by AHA’s CPR Facts and Stats report, which shows early CPR can double or triple survival odds after cardiac arrest.
Getting shocks on board: defibrillation timing and choreography
Rapid rhythm analysis and early defibrillation remain among the most effective interventions for shockable rhythms in out-of-hospital cardiac arrest. Teams should coordinate clearly: one provider maintains compressions, another charges the defibrillator and delivers shock, then immediately resumes compressions without delay. These teamwork and timing principles are core components of ACLS certification training, which expands on basic life support by adding rhythm recognition and medication protocols. Pauses for pulse checks or repeated rhythm checks should be avoided. Device choreography often fails under stress; pre-planning and role assignment reduce delays. High-quality CPR combined with prompt defibrillation improves odds of neurologically intact survival.
Using feedback devices and debriefs to hard-wire performance
Real-time audiovisual feedback devices help crews monitor compression depth, rate, and fraction, enhancing compliance with guidelines. After any cardiac arrest call, structured debriefs reviewing monitor data identify pauses or performance gaps. Those reviews guide micro-goals for improvement, such as cutting pause durations or achieving optimal compression fraction. Agencies that embed feedback and continuous quality improvement often see better survival rates. The 2025 AHA Guidelines for CPR and ECC update underscores that consistent post-event debriefing correlates with higher resuscitation success across EMS systems.
Short, realistic scenarios to practice before summer
Crews should run short (10–15 minute) scenario drills simulating realistic summer emergencies — for example, cardiac arrest at a crowded pool, RV park, or festival. These drills emphasize rapid initial assessment, seamless compression-AED choreography, minimal pauses, and immediate resumption of compressions. Training should incorporate distractions (bystanders, noise, limited space) to simulate field conditions. Tracking performance metrics (rate, depth, pause duration, time to first shock) allows objective evaluation and improvement over time.
Skill #2: Airway and ventilation – mastering BVM before chasing the tube
Why modern evidence puts BVM back in the spotlight
The 2023 evidence-based guideline for prehospital airway management from the National Association of State EMS Officials re-evaluated airway approaches. This report reviewed bag-valve-mask (BVM), supraglottic airway (SGA), and endotracheal intubation (ETI) for cardiac arrest, medical emergencies, and trauma. The analysis found that in many cases, well-executed BVM provides outcomes comparable to invasive airways. For many calls, BVM remains the most reliable first option. Crews should refine foundational ventilation skills before focusing on advanced airway tools.
Mask seal, positioning, and two-rescuer BVM techniques
Crew members should master mask-seal techniques and airway positioning (head-tilt/chin-lift or jaw-thrust when spine injury suspected). They must avoid leaks, over-ventilation, or inadequate tidal volumes. Two-rescuer BVM improves mask seal and ventilation quality, with one provider focusing solely on seal and another on ventilation. Regular practice using manikins or simulation tools ensures providers can deliver effective BVM ventilation under pressure. Use of capnography (if available) helps confirm effective ventilation and guide adjustments.
Advanced airway use: when it helps, when it hurts
Agencies with rigorous training and continuous quality improvement may employ advanced airways such as SGAs or ETI. But ETI only delivers advantages if providers maintain high success rates and minimize interruptions. Overemphasis on early intubation has correlated with prolonged scene times and worse outcomes in hemorrhagic trauma cases. Pediatric cases demand special attention because airway anatomy and ventilation needs differ markedly from adults. Providers who maintain PALS renewal certification ensure they stay current on pediatric rhythm interpretation and emergency care updates.
Airway decisions in bleeding trauma – circulation before airway
Modern prehospital trauma philosophy often prioritizes hemorrhage control and rapid transport over early airway intervention in severely bleeding patients. This “circulation-first” mindset reduces delays to definitive care. Crews should assess blood loss severity and decide whether delaying advanced airway and focusing on hemorrhage control yields better survival odds. Summer trauma scenes (traffic collisions, water accidents, falls) often produce severe bleeding — this skill-set proves critical.
Skill #3: Catastrophic hemorrhage control and shock-first trauma thinking
What current hemorrhage-control statements actually say
The NAEMSP joint position statement emphasizes that uncontrolled bleeding remains a leading cause of preventable prehospital death. The guideline stresses immediate identification of life-threatening bleeding and use of direct pressure, tourniquets, wound packing or hemostatic agents. Early intervention by trained EMS personnel dramatically improves outcomes in trauma patients.
Tourniquets: early, effective, and safer than many providers still think
Well-applied tourniquets on major extremity hemorrhage significantly improve survival with low risk of severe complications. A 2024 study published on PubMed confirmed that early tourniquet use yields high hemorrhage-control success and minimal complications. Crews may hesitate due to concerns about pain or limb loss, yet evidence rejects those fears when tourniquets are applied correctly. Application should start as soon as major bleeding is identified, with time marked and reassessed during transport.
Wound packing, junctional bleeding, and hemostatic dressings
Not all bleeding injuries allow tourniquet application. Junctional wounds — groin, axilla, torso — often require wound packing and direct pressure. Hemostatic dressings or agents may supplement packing when protocols permit. Crews should train to locate bleeding origin, apply firm packing pressure, and secure dressings even through patient movement. Realistic scenario drills — for instance, falls at rocky terrain or boating accidents — help build confidence and competence under stress.
Putting <C>ABCDE into practice on chaotic summer scenes
Trauma protocols like <C>ABCDE prioritize catastrophic hemorrhage before airway and breathing. Applying that in crowded summer scenes (pool incidents, festival injuries, water sport accidents) demands rapid assessment and decisive hemorrhage control. Crews must balance speed and thoroughness, even when bystanders, noise, or environment distract them. Practice scenarios combining hemorrhage control, airway decisions, and rapid extrication help crews internalize the correct priorities.
Skill #4: Early recognition and pre-alert for stroke, STEMI, and sepsis
Stroke: scales, large-vessel suspicion, and prenotification
Accurate prehospital identification of stroke plus prenotification to receiving hospitals improves door-to-treatment times and patient outcomes. Recent EMS research underscores the value of using validated stroke scales and transferring last-known-well times. Agencies with dispatcher or EMS-level training report faster recognition and shorter delays. Dense summer populations near beaches or crowded venues may raise risk for delayed recognition — crews should review stroke scales before the season begins. EMS-hospital coordinated protocols smooth transitions and accelerate definitive care.
STEMI: prehospital 12-lead ECG from capture to cath-lab activation
Prehospital acquisition of 12-lead ECGs and rapid transmission to hospitals enables early cath-lab activation and reduces door-to-balloon times. The AHA STEMI Systems of Care report demonstrates that coordinated EMS-hospital networks significantly improve survival for myocardial infarction patients. EMS providers should keep ECG equipment maintained, ensure clean signal acquisition even under bright sunlight or movement, and communicate findings clearly. Summer calls often involve exertion-related chest pain or dehydration — crews must remain vigilant for atypical symptoms. Agencies should audit metrics such as proportion of chest pain calls with ECGs and time from EMS contact to ECG completion.
Sepsis screening in a hot, busy environment
Hot weather and dehydration can mask or mimic early sepsis, especially in elderly or chronically ill patients. EMS crews should apply simple sepsis screening tools: check vital signs, mental status, signs of infection, and suspected source. Early recognition and pre-alert to hospital teams improve time to antibiotics and sepsis care. Providers must resist dismissing sepsis as mere heat exhaustion or dehydration — thorough assessment saves lives as much in summer as any other season.
The time-critical chain: dispatch, EMS, and hospital working as one
Timely interventions for stroke, STEMI, or sepsis require coordination from dispatch to hospital handoff. Dispatchers trained to recognize stroke or chest-pain calls shorten dispatch-to-EMS time. EMS crews capturing ECGs or stroke-screen data and pre-alerting hospitals help ED teams prepare. Clear, concise radio reports must include onset times, mental status, and interventions given. Agencies should run joint drills involving dispatch, EMS, and hospital staff before busy summer to test readiness.
Skill #5: Scene size-up, primary assessment, and handoff that prevent “quiet” deaths
Structured scene size-up that works in real life
Every scene demands safety assessment, understanding mechanism or illness cause, counting patients, and evaluating resources needed. Good scene size-up reduces risk for providers and patients alike. Summer emergencies often occur in challenging environments: beaches, camps, crowded festivals, roadways. Rapid, methodical assessment helps identify hazards, potential victims, and critical needs before treatment begins.
Primary assessment focused on life threats, not just checkboxes
Primary survey should identify life threats in airway, breathing, circulation, disability, and exposure. Where massive bleeding exists, crews should apply hemorrhage control first under trauma protocols. Structured assessment allows earlier detection of hidden threats — internal bleeding, spinal injury, hypoxia, or shock. Providers should remain alert to subtle signs in noisy or chaotic scenes and avoid assumption-based neglect.
Avoiding tunnel vision when everyone is shouting
High-stress scenes often overwhelm EMS crews with distractions: bystanders, noise, family, environmental hazards. Teams must avoid focusing solely on obvious injuries while missing subtle but life-threatening issues. Assigning roles, verbalizing observations, and maintaining periodic reassessment help preserve situational awareness. Crew communication and structured teamwork reduce errors from emotional stress or chaotic scenes.
Handoff tools (MIST, SBAR) that preserve critical details
Structured handoff methods like MIST (Mechanism–Injuries–Signs–Treatment) or SBAR (Situation–Background–Assessment–Recommendation) ensure continuity of care at hospital arrival. These tools help transmit vital information: injury mechanism, interventions applied (tourniquet, ventilation), time of onset, vital signs trends. Precise handoff enables ED clinicians to pick up where EMS left off without duplication or delay. Agencies should practice handoff drills regularly, encouraging clarity and completeness.
Turning evidence into a pre-summer practice plan
How fast skills decay – and what that means for training frequency
Recent EMS research confirms critical skills (CPR, airway, hemorrhage control) degrade within months without regular practice. Feedback devices or skill checks can reveal fallen performance. Many EMS systems rely on two-year recertification cycles — that leaves long gaps where performance drops. Periodic, focused refreshers before high-demand seasons such as summer help maintain readiness. Agencies should consider quarterly or seasonal drills rather than only formal recertification.
Studies from AHA and NAEMSP indicate that psychomotor skills in resuscitation and trauma care decline far sooner than certification cycles suggest. The table below summarizes documented decay timelines and suggested retraining intervals for key EMS competencies based on peer-reviewed and institutional data.
| Skill Area | Primary Source or Guideline | Documented Skill Decay Timeline | Recommended Refresher Interval | Key Notes / Study Highlights |
|---|---|---|---|---|
| High-quality CPR | AHA CPR & ECC Guidelines (2020–2025) | 3–6 months after training | Quarterly practice or monitored drills | Compression depth and fraction decline rapidly without feedback devices or debriefing. |
| Bag-valve-mask ventilation | NASEMSO Prehospital Airway Management EBG (2023) | 4–8 months for measurable degradation | Semi-annual simulation or airway lab | Technique errors and leak rates rise quickly without hands-on repetition. |
| Hemorrhage control (tourniquet, packing) | NAEMSP Joint Position Statement (2023) | 6–9 months post-training | Annual trauma skills validation | Providers forget pressure application technique and device placement sequence. |
| Stroke & STEMI recognition | AHA Stroke and ACS Systems of Care | 4–6 months for screening accuracy decline | Bi-annual scenario reviews | Early recognition accuracy drops as diagnostic cues fade from memory. |
| Structured handoff & communication | National EMS Education Standards (2021) | Up to 12 months without formal refreshers | Annual competency review | Loss of format discipline (MIST/SBAR) leads to incomplete hospital transfers. |
Designing brief, high-yield drills around the “big five” skills
EMS leaders should build a pre-summer training calendar including four to six short scenario-based sessions covering CPR/AED, BVM airway, hemorrhage control, stroke/STEMI/sepsis recognition, scene assessment and handoff. Structured paramedic training programs reinforce these scenarios through clinical rotations and advanced simulation, bridging classroom skills with field performance. Each session should include realistic environment stressors: noise, limited space, bystanders. Use manikins, realistic moulage, bleeding simulators, and full equipment setups. Post-drill debrief should review performance data, highlight strong and weak points, and set measurable improvement goals.
Using local QA data to target weak spots before summer
Agencies should analyze their own EMS call data to identify patterns: cardiac arrest outcomes, CPR quality metrics, hemorrhage control use, time-to-ECG for chest pain, stroke prenotification rates, scene times, and handoff completeness. Identified deficiencies provide focused areas for pre-summer drills. Tracking improvement over time strengthens system readiness and highlights training value. Medical directors and QA officers should lead data-driven planning and continuous quality improvement cycles.
Carrying these five skills into every season
Building a culture of continuous skills maintenance
EMS agencies should embed regular micro-training and debrief sessions rather than depend solely on large-scale courses. Peer-to-peer teaching, crew-led simulations, and rotating leadership encourage shared responsibility for competence. Agencies should invest in feedback devices, simulation kits, and simple tracking tools. A strong culture of continuous improvement fosters readiness for peak periods — summer or otherwise — and supports consistent high-quality care.
Quick-reference checklist for crews heading into a busy season
Crews should carry a laminated checklist summarizing core skill domains and performance targets: CPR rate/depth/CCF, BVM readiness, hemorrhage control equipment check, ECG and stroke screen readiness, scene assessment and handoff format. They should review that checklist at start of each shift or weekly. That routine promotes consistency and mental preparedness throughout the season. Maintaining readiness through all months ensures better patient outcomes and saves lives.
Frequently Asked Questions
What exactly counts as “high-quality CPR”?
High-quality CPR meets guidelines: 100–120 compressions per minute, depth of at least 2 inches in adults, full recoil, no excessive ventilation, and compression fraction above 80%. Teams must minimize interruptions and ensure proper coordination.
When should EMS choose BVM over advanced airway devices?
EMS should start with bag-valve-mask ventilation in most situations. Advanced airways (supraglottic or endotracheal) may follow only when needed and only if crews maintain continuous training and high success rates.
Why focus on hemorrhage control first in major trauma?
Uncontrolled bleeding causes many preventable prehospital deaths. Swift hemorrhage control — using tourniquets, packing or pressure — often proves more time-sensitive than immediate airway or IV interventions.
How does early recognition of stroke, STEMI or sepsis change patient outcomes?
Identifying stroke, STEMI, or sepsis early allows hospitals to prepare and activate timelines for reperfusion or sepsis treatment faster. EMS prenotification shortens delays and improves chances of good outcomes.
How often should EMS teams rehearse these core skills?
Agencies should run brief, high-yield drills every few months, ideally before high-demand seasons. Frequent refreshers help prevent skill decay and maintain readiness year-round.

Lisa VanderMeulen brings over 15 years of field experience as a licensed paramedic and firefighter in Florida. She currently serves as a Lieutenant with the Lehigh Acres Fire Control & Rescue District and as Dean of Ricky Rescue Training Academy, where she oversees curriculum development for EMT and fire service education.
Lisa holds an Associate of Science in Emergency Medical Services Technology from Florida SouthWestern State College and advanced certifications from the Florida Bureau of Fire Standards & Training, including Fire Officer II, Fire Instructor II, and Incident Safety Officer. Her licensure as a paramedic is backed by the Florida Department of Health.
In addition to her teaching and command roles, she actively serves on safety committees, community outreach programs like Fire Prevention Week and Pink Heals, and holds leadership positions within IAFF Local 1826.